Author: Lisa Spriet, Registered Dietitian
Being told you have a fatty liver can feel confusing! Are you unsure what your next steps should be? Can changing the way you eat help? Overwhelmed by all the acronyms you’ve come across? Well, fear not, because we understand what you’re going through and are here to help explain! This blog will take you through the basics of fatty liver, including various terms and lab values, as well as help you get started on reversing fatty liver. Let’s dive in!
What Is Fatty Liver?
The liver naturally has a small amount of fat in its cells. This is normal. But when there is too much fat stored in the liver, it becomes a problem. You have Fatty Liver when more than 5% of your liver is fat. Having this condition puts your liver at risk of getting more serious injuries, like liver inflammation or scarring, which can lead to liver failure. The term Non-Alcoholic Fatty Liver Disease (or NAFLD) refers to fatty liver that is not due exclusively to unhealthy alcohol use, which is another cause of fat accumulation in the liver.
This is the most common liver disease in Canada, affecting 20% of Canadians. The liver is responsible for processing all foods and fluids you consume. It may help to think of your liver as a waste removal plant attached to the plumbing system. Fat accumulation is the equivalent of sludge building up in a plumbing system, and like a plumbing system, this build-up interferes with processing.
Why Do People Get Fatty Liver?
As mentioned, unhealthy alcohol use is one cause, but in terms of NALFD, there are many factors that can contribute to Fatty Liver. Among the most common are Habits and Body Factors. Let’s explore those further:
Habits
- Drinking sugar-sweetened or high-sugar beverages (Juice, Soda, Pop, Energy drinks) on a regular basis (ie. daily)
- Eating too many refined carbs in your diet, such as cookies and baked goods, and processed grains such as sugary cereals and white bread products (ie. daily)
- Unbalanced eating habits, such as having very large meals
Body Factors
- Having large amounts of belly fat, also known as visceral fat
- Obesity
- Problems with gut health
- Insulin resistance, pre-diabetes or diabetes
- Metabolic syndrome (high blood pressure, cholesterol, and blood sugar, large waist circumference, high lipids in the blood)
Regarding habits and body factors, many of these go together, for example eating too many refined grains on a daily basis can lead to belly fat, high blood sugar levels and fatty liver.
The Development Of Permanent Liver Disease:
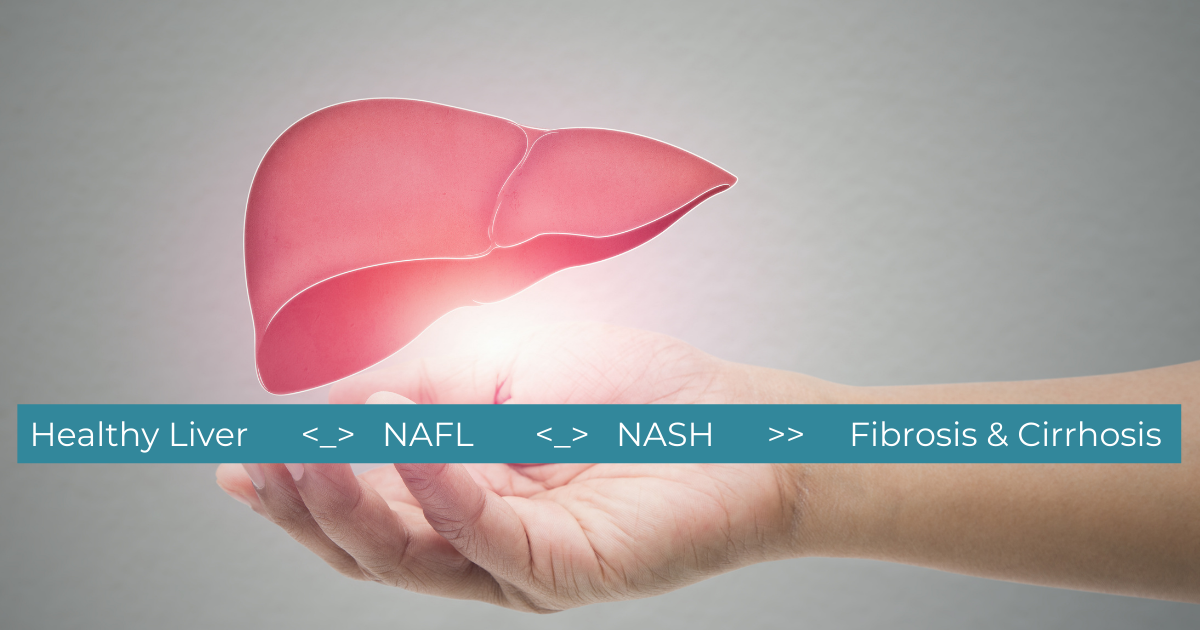
Without intervention for Fatty Liver, the liver fat can become inflamed and damage liver cells, progressing the disease to Non-Alcoholic Steatohepatitis (NASH). Long-term heavy drinking leads to similar symptoms to NASH, but NASH develops without alcohol abuse.
If fatty liver is not corrected and progresses, NASH can turn into Fibrosis, where the buildup of scar tissue makes it difficult for blood circulation in the liver, meaning the liver then cannot do its job. If this continues, liver Fibrosis can lead to Cirrhosis (excessive scarring interfering with the liver’s function) and liver failure. Once in liver failure, the only option is a liver transplant, which is an invasive and not always successful surgery.
With treatment, NAFL can be reversed back to a healthy liver, and NASH can reverse back into NAFL. Fibrosis and Cirrhosis, on the other hand, are permanent and cannot be reversed. For this reason, identifying and treating fatty liver before it progresses is of utmost importance!
How Do You Test For Fatty Liver?
Currently, there are two ways to assess fatty liver: blood tests (liver function and liver tests for inflammation) and FibroScan or ultrasound.
- Blood Tests:
a) Testing for inflammation and liver injury – these are the enzymes that are measured in blood:
- Alanine aminotransferase (ALT or SGPT)
- Aspartate aminotransferase (AST or SGOT)
- Gamma glutamyl transferase (GGT)
b) If cirrhosis is suspected, tests to see how your liver is functioning may also be included:
- Bilirubin levels to check if your liver is properly breaking down waste
- Albumin is a protein made by the liver and low levels are often seen in damaged livers
- Prothrombin is another protein made in the liver that shows blood clotting. It’s also known as the International Normalized Ratio (INR).

2. FibroScan
FibroScan (also called liver elastography) uses ultrasound waves to find the degree of fibrosis or scarring in your liver. This is a non-invasive procedure that is painless and takes about 10 minutes. It gives an accurate measure of the amount of fat accumulation, as well as potential scarring. Having this test done is important as blood tests don’t always give an accurate measure of fat accumulation in the liver.
What Are People With Fatty Liver Told About These Tests?
Both ALT and AST are often done as part of routine lab work. If your levels are elevated, your doctor may use this information alone to tell you that you have fatty liver.
They may also send you for an ultrasound or FibroScan to confirm fatty liver, as well as the severity of fatty liver.
Lastly, if fibrosis is suspected, your doctor may tell you your ‘FIB-4’ score, which is an estimate of liver fibrosis.
What Do I Do If I Have Fatty Liver? Medication? Lifestyle?
While there are always advances in medicine, there is no medication that specifically targets reducing liver fat. Currently, lifestyle interventions, including healthy eating and regular physical activity, are the only proven ways to reverse fatty liver disease.
In terms of lifestyle, here are some key factors:
- Eliminate high-sugar foods and beverages, as well as processed carbohydrates
- Limit alcohol intake
- Increase ‘whole foods’ such as whole vegetables and fruits, whole grains, legumes, to increase fibre and antioxidant intake
- Include adequate protein from plain, low-fat dairy and lean fish and poultry and eggs
- Increase omega-3 intake and decrease saturated fat intake
- If you’re overweight, try to lose 5-10% of your body weight
- Be active every day, aiming for 30-60 minutes of activity on most days of the week
By following these recommendations, many of our clients have seen complete resolution of fatty liver within 3-6 months, depending on the degree of fatty liver. You can download a program overview on our Liver Health page, or take a self-paced course to learn more.
What Is Our Approach To Helping Clients With Fatty Liver?
With liver disease, there’s a lot to keep track of: your diet, your current blood lab values, your goals, your medications, your fitness, and many other health-improving factors.
A dietitian can help you by:
- Dietary counselling
- Making a meal plan fit to your specific needs with what to eat, and what to avoid for liver health
- Advice on how to eat better, how to grocery shop, how to read nutrition labels, useful supplements, and what to eat that fits with your lifestyle or even when you’re eating out
- Weight loss if and when appropriate
- Keep you on track, including goal setting and overcoming barriers
- Knowing the process
- Being familiar with what you’re going through and being able to give advice specifically tailored to you on what to do
- Interpreting what your lab values mean and helping you understand all that jargon!


Personalized Liver Health
Plans & Supplements
Repair The Damage And Start Improving Your Liver Health.
Choose a single session, an express or a comprehensive program.


We stumbled over here different web address and thought I may as well check things out. I like what I see so now i’m following you. Look forward to looking at your web page yet again.
Hi, Where are youi locaterd? Thanks.